Action Is Needed Soon to Ensure More Affordable Health Insurance Coverage
May 16, 2022 / by Christina Cousart and Maureen Hensley-Quinn
Without Congressional action in the coming weeks to extend the American Rescue Plan Act’s (ARPA) enhanced marketplace tax credit, the gains made in the last year to increase affordability and enrollment for millions could be temporary. The resulting increased cost of coverage will hit families already struggling to stretch their finances to make ends meet in the face of climbing inflation. (For more information about ARPA’s coverage gains see NASHP’s infographic on how ARPA is making coverage affordable and accessible to millions of consumers).
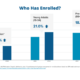
In 2021, ARPA made historic investments to increase the affordability of health care coverage drawing a record number of enrollees to the health insurance marketplaces, including nearly 3.1 million individuals who newly enrolled this year including significant growth in enrollment across young adults, rural and older adult (55+) populations. However, these investments are currently set to expire at the end of this year leaving the health insurance marketplaces to begin contingency planning for the next open enrollment period. (For more information about how the loss of ARPA tax credits will impact consumers see: State-Based Marketplaces Say Many Will Close Coverage If Premium Assistance Expires.)
Premium Rate Considerations Are Underway
Insurers are already planning their portfolio of 2023 health plan offerings. Proposed rate filings will begin to be issued this month and without the enactment of an extension of ARPA tax credits, insurers are left to assume the enhanced tax credits will end per existing law. As a result, insurers will likely anticipate consumers disenrolling due to higher costs, worsening the plan’s risk pool and leading the insurers to propose increased premiums. This effect may be exacerbated by estimated increases in health care spending expected in the next year. For example, in Vermont, one of the first states to issue preliminary rate filings this year, insurers are seeking approval for double-digit premium increases. Combined, the enhanced tax credit lapse and increased premiums will significantly increase costs for consumers, resulting in disenrollments.
Final rate filings are due by August 17, with some states imposing earlier deadlines for their insurers. Proposed and final rates are usually publicly posted giving consumers and other stakeholders an indication of what to expect for the upcoming year. Once rates are finalized, little can be done to change agreed-upon premiums, as marketplaces and insurers must immediately prepare for enrollment into the plans that have been approved for the year. In addition, notices to consumers will be sent as early as September with these premium rates. If rates are significantly higher, consumers may find coverage unaffordable and opt to be uninsured.
Marketplace Operational Changes Planned for This Summer
Health insurance marketplaces will need to make major systematic changes if ARPA’s tax credit enhancements lapse. These will include significant changes like updating eligibility criteria, cost calculators, and revamping “plan mapping” tools designed to guide consumers to comparable options in the case their former plan is no longer offered. State marketplace officials must make decisions now about where to prioritize their limited resources – both funding and staff time – in preparing for the next open enrollment period. Can they devote resources to further enhancing the consumer experience? Or do they need to begin dismantling the systems and policies that support the enhanced tax credits? The longer federal decisions are delayed, the more costly they become to implement.
State-based marketplaces are also strategically considering how best to mitigate sticker shock when enrollees begin receiving renewal notices with updated premiums that will start as early as September. Currently, marketplaces are expecting to make robust investments in outreach and educational campaigns to explain the premium changes, promote active shopping, and encourage customers to retain their coverage for the next year. If Congress acts to extend the enhanced tax credits after initial renewal notices are sent, marketplaces will need to redouble efforts to clarify confusion in the middle of their already busy enrollment seasons.
Anticipated Medicaid Unwind Adds to Complexity
The uncertainty of the enhanced tax credits extension is further complicated by the unknown but the eventual transition of millions of individuals from Medicaid to marketplace coverage. This transition is part of changes expected once the federal public health emergency ends and states will no longer be required to maintain Medicaid eligibility for all who are currently enrolled. Of the up to 14 million estimated to be disenrolled from state Medicaid programs; it is estimated nearly 5 million could qualify to purchase subsidized coverage through the marketplaces.
State-based marketplaces are actively coordinating with their state Medicaid agencies on strategies to ease the transition of those moving between programs. However, individuals losing Medicaid coverage may not be able to afford marketplace coverage without the enhanced tax credits. ARPA’s subsidy enhancements ease the transition between programs, especially for the lowest-income individuals (those making up to $20,385 per year) who currently qualify for $0 marketplace benchmark plans. If the enhancements are not extended, these individuals could be required to pay up to $70 per month for a benchmark plan, likely leading many to drop coverage even if they could successfully transfer to marketplace coverage.
Although the next open enrollment period officially begins in late fall, decisions are being made now to prepare for it. Health plans are working to ensure there are coverage options available and they are generally using current law to predict consumer action to build premiums that will likely be more costly. States must prioritize investments in policy, systems, and communications now to be prepared and there will be costs to duplicating that work if federal policy changes later. In addition, consumers require clarity — to avoid confusion and create an affordable glidepath to coverage. Because of this — immediate congressional action regarding the extension of ARPA’s affordability enhancements is needed for states, marketplaces, and insurers to deliver the best possible coverage environment for consumers. NASHP will continue to monitor and report as states evaluate the impact of ARPA on their marketplace consumers and plan for the next open enrollment period.
How ARPA’s Premium Affordability Measures Impacted Consumers1
Changes made under APRA both enhanced the amount of tax credits available to help individuals and families purchase coverage and imposed a first-time cap on the proportion of income families are required to pay for coverage. In practice, these changes meant that:
- A family of four making $41,625 per year went from paying $1,723 to qualifying for free coverage for the year.
- Annual costs for a family of four earning $69,375 decreased from $5,779 to $2,775.
- An individual making $55,000 per year went from paying an average of $5,256, to having costs capped at $4,675.
1Based on 2022 federal poverty levels and assumes purchase of benchmark a benchmark plan. Average payment based on 2022 benchmark premium data as reported by the Kaiser Family Foundation.


 For individuals living with complex, often chronic conditions, and their families, palliative care can provide relief from symptoms, improve satisfaction and outcomes, and help address critical mental and spiritual needs during difficult times. Now more than ever, there is growing recognition of the importance of palliative care services for individuals with serious illness, such as advance care planning, pain and symptom management, care coordination, and team-based, multi-disciplinary support. These services can help patients and families cope with the symptoms and stressors of disease, better anticipate and avoid crises, and reduce unnecessary and/or unwanted care. While this model is grounded in evidence that demonstrates improved quality of life, better outcomes, and reduced cost for patients, only a fraction of individuals who could benefit from palliative care receive it.
For individuals living with complex, often chronic conditions, and their families, palliative care can provide relief from symptoms, improve satisfaction and outcomes, and help address critical mental and spiritual needs during difficult times. Now more than ever, there is growing recognition of the importance of palliative care services for individuals with serious illness, such as advance care planning, pain and symptom management, care coordination, and team-based, multi-disciplinary support. These services can help patients and families cope with the symptoms and stressors of disease, better anticipate and avoid crises, and reduce unnecessary and/or unwanted care. While this model is grounded in evidence that demonstrates improved quality of life, better outcomes, and reduced cost for patients, only a fraction of individuals who could benefit from palliative care receive it. 























































































































































